Applications of Placental Tissue in Dermatology: Mohs Micrographic Surgery
The Merits of Placental Tissue in Wound Care
Use of placental tissues has been recorded for over a century, beginning in 1910 as an allograft during skin transplantation procedures.1 Today these tissues are used in a variety of applications including ophthalmology, burns, skin wounds, and chronic ulcers.1 There is a growing body of scientific and clinical evidence detailing the characteristics and effectiveness of placental tissue in wound care, with lower extremity wounds being the most common wound type to be treated with placental-derived tissue products. While lower extremity wounds have been a focal point of placental tissue experimentation, interest in other applications is growing. One space where placental-derived tissue products are growing in popularity is in post-operative care following Mohs micrographic surgery (MMS) procedures.2,3
Mohs Micrographic Surgery for the Excision of Nonmelanoma Skin Cancers (NMSC)
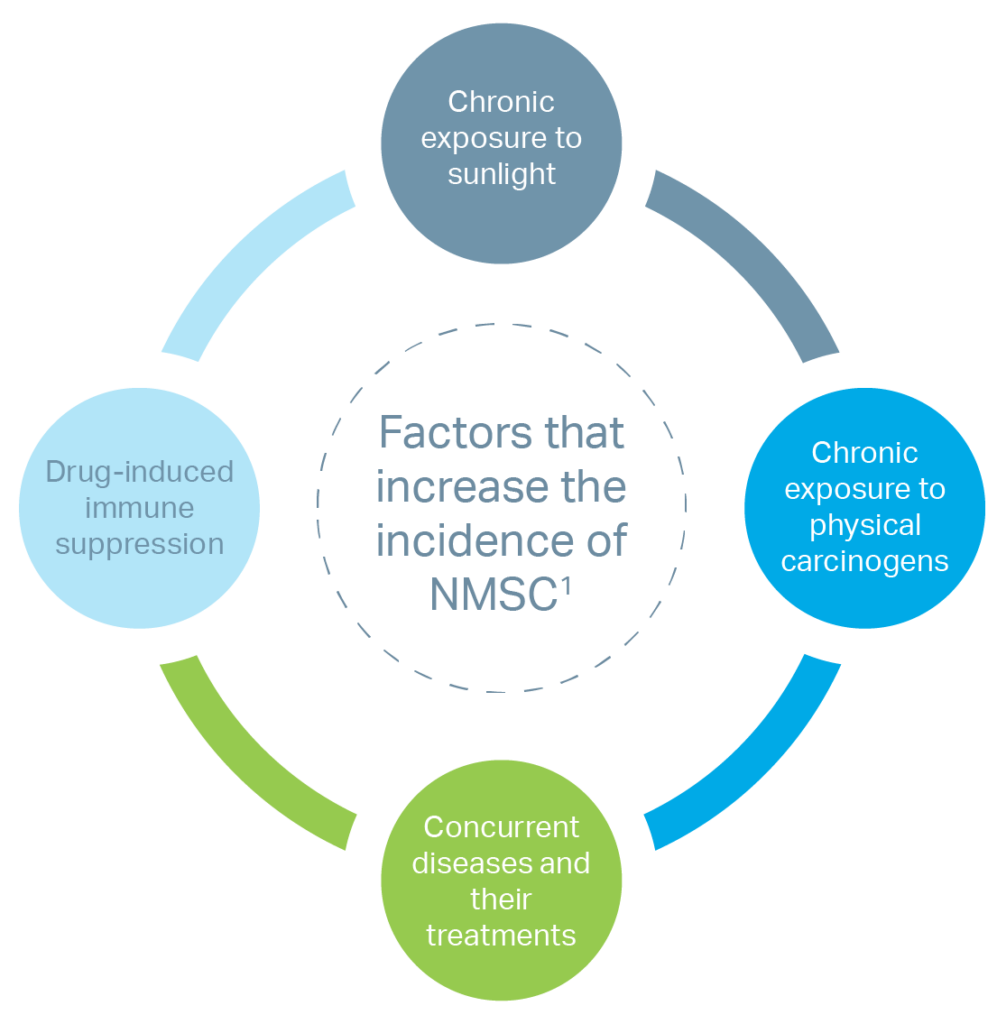
In general, the incidences of both melanomas and NSMC are increasing worldwide due to multiple factors.4 For the purposes of this post, we’ll focus on NSMC and the procedure that can be used to treat them.
NSMC can be divided into 3 main groups: basal cell carcinomas (BCC), squamous cell carcinomas (SCC), and Merkel cell carcinomas (MCC).4 Epidemiological surveys indicate a recent significant surge of NMSC in the elderly population.5 As many as 80% of all new cases of NMSC are occurring in patients over 65 years of age.5 These types of skin abnormalities can require repeat surgical intervention to achieve adequate removal of the abnormal tissue while preserving the functional and aesthetic aspects of the remaining skin.5
One of these forms of intervention is Mohs micrographic surgery, or MMS! MMS is a multi-step, same-day procedure, requiring local anesthetic, that is typically performed in the outpatient setting.6 The process begins with the removal of any visible abnormal tissue. The tissue is then frozen and sectioned for analysis in a laboratory within the clinician’s office. The surgeon will examine the sections and note any locations where abnormal tissue remains. If abnormal tissue persists in the sample, the surgeon will repeat the procedure until tissue margins are confirmed to contain no abnormal tissue.
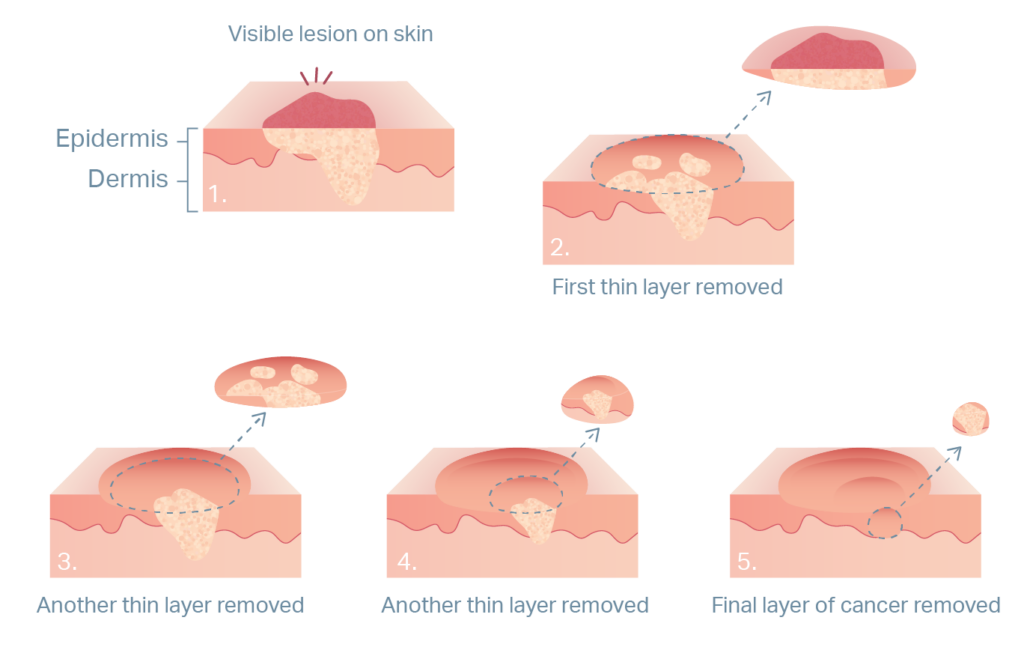

MMS procedures are currently the most effective method of eradicating BCC and SCC, with a 5-year cure rate of 99% in patients that have had a BCC removed.6 Another advantage is that MMS spares healthy tissue from excision, which is paramount when treating NMSC around the eyes, ears, nose, or mouth.6
Based on the size and location of the wound left from the MMS procedure, the surgeon will select the most appropriate wound repair technique. Smaller wounds may be left open to heal on their own, this is referred to as secondary intent. Larger and deeper wounds may require additional reconstructive options including stitches, skin flaps or skin substitutes.6,7
The Use of Placental Tissue-Derived Products in MMS Procedures
While highly effective at removing NMSC, MMS procedures can sometimes leave large surgical wounds. These wounds may require the creation of a rotation or advancement skin flap, which involves the manipulation of surrounding skin to cover the wound. Other solutions for these larger MMS-related wounds include skin substitutes.7 Scientists and clinicians have begun analyzing the effect of placental tissue-derived products on MMS-related wounds using small-scale studies, case series, and retrospective analyses.3,5,7 Evidence thus far has demonstrated advantageous benefits to using placental tissue-derived products in MMS-related wounds compared with the current standard of care procedures.3,5,7 Currently, the most apparent advantage to using placental tissue derived-products in MMS-related wounds is the ease of post-procedure wound care. With these products, patients can come into the office approximately once a week, depending on their clinician’s preference, for a dressing change and application of a new allograft. Conversely, traditional healing by secondary intent requires daily cleaning, dressing changes, and consistent attention.3,7 In a 2021 retrospective case-control study of a placental tissue-derived product compared with autologous tissue-based procedures, the placental tissue-derived product demonstrated a lower risk of infection and repeat operation.5 Additionally, wounds treated with autologous grafting reported a higher incendence of poor cosmetic outcome and requirement of scar revision than those treated with placental tissue-derived product.5 Additional studies have also reported that wounds treated with AM required fewer dressing changes than traditional SOC, resulting in a reduction of the discomfort caused by frequent dressing changes.3,7
As wound care continues to evolve and evaluate new treatments, it is clear that placental tissue-derived products can be a beneficial component of the treatment continuum for a variety of wounding scenarios including, but not limited to, wounds created by the MMS procedure. While the use of placental tissues in wound resolution is nothing new, we continue to see expanding evidence on just how useful these tissues can be.
For the latest updates on StimLabs, information on disease states that may create risk factors for chronic wounds, and non-medicinal educational patient tips, please follow StimLabs Unprocessed.
Disclaimer: Please note that the preceding text includes summaries from literature that in no way reflects any current product offerings or product claims provided by StimLabs LLC. The inclusion of this information within the text above is only for educational purposes and does not reflect the products, goals, or opinions of StimLabs, LLC as a company.
MKTG22-028 Rev 01
1. Dua, H. S., & Azuara-Blanco, A. (1999). Amniotic membrane transplantation. The British journal of ophthalmology, 83(6), 748–752. https://doi.org/10.1136/bjo.83.6.748 2. Kogan, S., Sood, A., & Granick, M. S. (2018). Amniotic Membrane Adjuncts and Clinical Applications in Wound Healing: A Review of the Literature. Wounds : a compendium of clinical research and practice, 30(6), 168–17 3. Seaton K, Mullens D, Barr J, Hull E, Averitte R. Use of Amniotic Tissue-Derived Allografts Post-Mohs Micrographic Surgery: A Preliminary Study Assessing Wound Closure Rate. Wounds. 2021;33(7):185-191. doi:10.25270/wnds/2021.185191 4. Cives, M., Mannavola, F., Lospalluti, L., Sergi, M. C., Cazzato, G., Filoni, E., Cavallo, F., Giudice, G., Stucci, L. S., Porta, C., & Tucci, M. (2020). Non-Melanoma Skin Cancers: Biological and Clinical Features. International journal of molecular sciences, 21(15), 5394. https://doi.org/10.3390/ijms21155394 5. Toman J, Michael GM, Wisco OJ, Adams JR, Hubbs BS. Mohs Defect Repair with Dehydrated Human Amnion/Chorion Membrane. Facial Plast Surg Aesthet Med. 2022;24(1):48-53. doi:10.1089/fpsam.2021.0167 6. Bowen, G. M., White, G. L., Jr, & Gerwels, J. W. (2005). Mohs micrographic surgery. American family physician, 72(5), 845–848. 7. Lyons, A. B., Chipps, L. K., Moy, R. L., & Herrmann, J. L. (2018). Dehydrated human amnion/chorion membrane allograft as an aid for wound healing in patients with full-thickness scalp defects after Mohs micrographic surgery. JAAD case reports, 4(7), 688–691. https://doi.org/10.1016/j.jdcr.2018.03.015
share this article
















